Early childhood is a critical period that determines a person’s ability to reach his or her lifelong health, social, and economic potential. Comprehensive early childhood well-being—which consists of physical and mental health, cognitive functioning, and social and emotional development—has strong links to long-term outcomes such as educational attainment, annual income, and mental health. Research shows that there are significant economic benefits to ensuring young children receive the care they need. Therefore, a comprehensive early childhood health and education system is a crucial component of determining our nation’s future. In fact, one study found that every dollar invested in early childhood well-being has the potential to produce approximately $8 in returns for society.1 (Dive deep into early childhood wellbeing in this interactive.)
Stay current on your favorite topics
However, quality, access, and coordination of early childhood well-being programs and initiatives vary considerably from state to state. Many states spend their early childhood funds less efficiently than they could, and not all families have sufficient access to affordable, high-quality, development-oriented healthcare, childcare, and preschool. In 2015, almost two decades after the passage of the Children’s Health Insurance Program (CHIP), 5 percent of children did not have health insurance. That same year, more than half of three- and four-year-old children in the United States were not enrolled in preschool.2 And among programs that participated in states’ Quality Rating and Improvement Systems (QRIS), 30 percent of center- and home-based licensed childcare programs scored in the bottom tier, and fewer than 15 percent rated at the top of the scale.3 Minority and disadvantaged populations in particular lack access to affordable, high-quality services. In Los Angeles, for example, low-income communities and areas populated mostly by people of color face more severe shortages in access to licensed childcare than higher socioeconomic communities.4 Across the country, the poorest children attend significantly lower-quality prekindergarten (pre-K) programs, on average, than their wealthier counterparts.5 And African American, American Indian, and Hispanic children are far more likely to live in high-poverty areas.6
Research also suggests that children from low-income families are more likely to exhibit developmental delays, behavioral problems, and other disabilities than children from wealthier families. These adverse effects have a long-term detrimental impact on health, academic outcomes, and income earned later in life. One study of US children has shown that being in the top 10 percent of the distribution of attention-deficit/hyperactivity disorder (ADHD) symptoms nearly doubles the probability of repeating a grade and often leads to 8 to 10 percent lower math and reading test scores.7
These gaps have serious consequences. Studies indicate that the achievement gap for children from lower-income families is the largest before kindergarten. By the time a low-income child starts kindergarten, he or she can be two to three years of learning behind advantaged peers.8 Often, this gap persists until third grade—the point at which a child’s ability to read is highly predictive of overall future life outcomes.9
But all is not lost.
The role of states in improving early childhood well-being
State governments have a unique opportunity to improve the developmental trajectories of children. In fact, states distribute tens of billions of dollars in funding for programs that are central to early childhood well-being, including Medicaid, CHIP, Temporary Assistance for Needy Families (TANF), and Child Care and Development Fund (CCDF) partnership. They also control $8.5 billion in public pre-K funding. For example, in 2012, states provided pre-K to 30 percent of four-year-old children—more than twice as many children as Head Start.10 States also regulate the quality of these programs, and they have the data (and thus the visibility) on which services are provided and by what methods. For this reason, they increasingly play a critical role in connecting children and families with the suite of healthcare services, education services, and information required to ensure well-being.
Providing this assistance efficiently is not easy. To get it right, states could pursue an integrated, comprehensive approach linking health and social services and education programs. While many states have made strides toward increasing access to and improving the quality of early childhood programs in this way, overall performance still lags behind.
Currently, states and cities often struggle with integrating and coordinating services across the social safety net. For example, children receiving early intervention services may experience an interruption in support when transitioning to preschool or kindergarten, and care recommended by pediatricians is often not continued by a child’s daily caregiver in childcare or preschool.
Investments in health and education, then, may not achieve the same results as when they are effectively coordinated. In addition, data is fragmented across many stakeholders and systems, which makes it difficult for governments to measure performance and match outputs (the extent to which spending and services reach various child populations) to outcomes (the impact of these services on child well-being). This lack of coordination also affects how families are able to navigate the system—especially those with less education or limited English proficiency. As a result, children often miss out on available services.
States must ensure that all children receive the high-quality services and supports they need for their well-being from birth through age five. This means supporting their physical health, cognitive development, and social and emotional health (Exhibit 1). Reaching only a subset of children on a subset of these dimensions is simply not enough.

States can strengthen and expand 14 support elements (Exhibit 2). Success will require states to integrate their approach to all these services and increase efficiency in funding across the board. They can also ensure that families are able to navigate and make use of all services and supports, and that those services and supports actually produce results.

Successfully ensuring early childhood well-being is a humanitarian deed that has the possibility of producing significant financial returns. One estimate suggests that if all families were equally able to provide structured, nurturing, and stimulating environments as those with socioeconomic advantages, the United States could potentially realize more than $300 billion in annual budgetary, earnings, health, and crime benefits.11 However, no state has yet excelled at this comprehensive approach.
How states can help: Levers for a comprehensive approach to improving early childhood well-being
In this section, we list a set of example levers that states could focus on to make progress within the 14 dimensions—overall enablers, including physical health, cognitive function, and social and emotional health—described in Exhibit 2.
Improve overall transparency and coordination of the system
A precursor to progress is getting the state’s house in order by improving its coordination and cross-agency funding transparency.
Would you like to learn more about our Public Sector Practice?
Coordinate the provision of services across the delivery chain. To ensure that investments in health, education, and other social services achieve their desired effects, states could coordinate the provision of services across agencies. This coordination fosters continuity of services and supports. For example, the approach to health and development screenings conducted in primary care settings for infants can be carried through into early education settings.
To further enable continuity, states could take advantage of the benefits of cross-agency synergies and implement interagency tracking mechanisms or other tools. Exhibit 3 provides an example of an approach that one state has implemented to map treatment journeys, which gives state health and education leaders a better understanding of how to improve points of contact and implement a seamless care continuum across providers. In this example, the child, Jerry, was eligible for several services in various settings—but gaps in coverage and personal barriers (such as his mother’s anxiety) prevented him from receiving the care he needed. To help families access early childhood care, North Carolina uses a common metric to measure “warm handoffs” of children between services before age five. This approach ensures that the people involved in each step of a child’s care have the full context needed to support both the technical and “human” challenges he or she faces.

Eliminate cross-agency spending inefficiencies. States can identify inefficiencies in current spending to better aid in coordination. Funding for early childhood services is often fragmented across numerous federal and state sources, not all of which are exclusively dedicated to early childhood. Therefore, states could develop a common understanding of how funding works across agencies and programs and then use this information to facilitate regular cross-agency strategic planning and program implementation. This task can be difficult because the landscape of funding streams is often complex and siloed—for instance, different funding sources may have different eligibility requirements, quality standards, and required accountability restrictions and requirements.12
Exhibit 4 is an example of a map one state created to begin the process of establishing cross-agency collaboration on funding. In this state, approximately $3.7 billion was dedicated to early childhood programs in 2014, but an additional $12 billion in funding reached children from birth to age five in some way, such as through Medicaid, food stamps, and the Social Services Block Grant program. Because only a fraction of that money was devoted exclusively to children from birth to age five, the state was unable to precisely determine the sources and uses of many of its funds. Two states in particular assist in creating transparency for how programs and funds reach children: Georgia and Rhode Island. Both of these states assign unique identifiers to children at birth that follow them across all government services. This system allows these states to track services children receive, help identify outcomes associated with early childhood services, and create transparency in spending across agencies. The state of Washington went even further, creating a single agency to manage all programs related to early childhood, from education to health to support for working parents.

Improve access to and quality of healthcare for young children
Coordination across agencies enables states to commit more resources for ensuring access to and quality of healthcare. Two targeted measures can help states create maximum impact on outcomes in early childhood health.
Support informed decision making among families. To increase access to high-quality early healthcare programs, states could first focus on launching public-awareness campaigns about the importance of early childhood well-being, which services are available, information on qualified providers, and how families can access them. They can also concentrate on making connections with key outreach partners, such as pediatricians and homeless shelters, and designing or scaling aggregated online platforms. For example, in 2010 Colorado launched an online, searchable database through which families with children who have developmental delays or disabilities can seek early intervention providers and receive information on their credentials, licenses, and certifications. The database offers practical information, such as the providers’ years of experience working with young children, their methodologies (such as coaching and direct service), geographic service areas, availabilities, Medicaid acceptance, languages spoken, and contact information. It also provides the state with data on gaps in available services and recently informed an assessment of Medicaid distribution and providers throughout Colorado.13
Incentivize healthcare programs and providers to improve quality of care. To increase access to services for the most at-risk children, states could launch incentive programs, such as tying bonuses to the number of low-income children served through Medicaid. Such models have the potential to incentivize providers to allocate time and attention to both providing and following through on services. A program in California that ran from 2002 to 2004 tested the impact of multiple financial and nonfinancial incentives on provider quality. Five in seven plans increased the rate of well-child visits to 35 percent, from 4 percent.14
States can also focus on targeted training programs for key gatekeepers in the lives of children. For example, they can finance training for pediatricians to identify traits and behaviors that warrant screenings in early childhood checkups. Such early interventions have been shown to work. One program has nurses visit first-time, at-risk mothers at their homes during pregnancy and for the first two years of their child’s life. The program produced “sizable, sustained effects” on important child outcomes, including reduced trauma and improved cognitive and academic outcomes.15
Improve access to and quality of early education
State investment in early education can be an important component of improving the overall educational success and, eventually, future employment and earnings of children. Extensive evidence points to the ability of high-quality preschool to narrow the achievement gap and give at-risk children a better chance at success later in life.16 Below are two primary actions that can put states on the right track to improving early childhood education.
Build early education infrastructure and capacity. One way to expand access to early childhood education is ensure states have adequate infrastructure and capacity—that is, facilities and talent. In building infrastructure, states could concentrate on expanding access for at-risk children without sacrificing quality—for example, by dramatically cutting per-child funding to serve more children. New Jersey struggled with having enough space in public schools to provide state pre-K but solved the problem by subcontracting with high-quality, licensed childcare providers.
Increase early education quality through training, high standards, and incentives. States can work toward higher-quality early childhood education in three ways:
First, they can develop a strong foundational approach to increase training and learning among early childhood caregivers and educators. For example, states can mandate time for continued education through evidence-based professional development, as well as setting minimum education requirements for pre-K teachers. They can also take cues from best practices across the country. In 2016, Pennsylvania awarded grants to community colleges, state colleges, and universities that together aligned 300 early childhood education courses with the state’s core knowledge competencies.17 In Illinois, an online portal connects family childcare professionals and features more than 75 resources that provide high-quality care and meet the requirements for QRIS and family childcare credentials. In addition, the site offers videos, webinars, reports, handouts, and more information on topics such as child development, best practices, and wellness. More than 50 providers signed up in the first two weeks after the portal launched.18
Second, states can raise the bar by setting clear definitions and standards of quality. Many states implement a QRIS, but not all ensure that they track the quality indicators that are most highly predictive of improved health, cognitive, and social–emotional development of young children. Examples of successful quality measures include the Classroom Assessment Scoring System (CLASS), a metric used by only 29 percent of center-based programs and 17 percent of home-based programs across the country participating in a QRIS.19 At least ten states now include CLASS in their QRIS, and it is required for all Head Start programs. Louisiana uses CLASS to evaluate all state-funded preschools and licensed childcare centers, an approach that has transformed the conversations families have in their communities about how they choose where to send their children for education.
Third, after developing evidence-based quality standards for early care and education, states can incentivize programs to improve on those dimensions of quality. For example, two-thirds of states currently create tiers for per-child, state-funded reimbursement rates, tying them to measured quality of care.20 This mechanism provides both a road map and an incentive for programs to target improvement on the indicators that matter most for childhood development. Minnesota’s Early Learning Scholarship program, for example, provides scholarships to low-income families to pay for early care and education from a selection of state-approved providers. To qualify for this program, providers must achieve a three- or four-star rating (out of four) in the state’s Parent Aware ratings system—directly incentivizing providers to raise quality of care and education to better attract parents.21
Sample approach and objectives of a transformation effort
With these levers in mind, we believe three phases could improve the health, education, and overall well-being of children: identify what the state is spending and the services it provides to improve early childhood well-being; develop a comprehensive, cross-agency plan for improvement; and implement pilot improvement efforts, scaling those that are most effective (Exhibit 5).

Phase 1: Lay the groundwork for success
Understand current levels of services and spending. Map out the full suite of childhood well-being services that health and education agencies provide, as well as other federal and state funding mechanisms for different services. Distill the braided nature of funding (that is, what funding exists and from what sources) to illuminate how the current funding structure may lead to misalignment or inefficiencies across agencies and programs. Consider preparing for the challenges of identifying the landscape of funding and services by finding special capacity for the task, such as appointing a steering committee.
Evaluate the extent to which spending and services reach various subgroups of children and families. Highlight any gaps or inefficiencies in funding and services between advantaged and disadvantaged children and families. Prioritize at-risk subgroups, including teen parents, families in poverty, single parents, parents with little education, non-English-speaking students or parents, unemployed parents, families with high rates of residential mobility, and large families. Key analyses might include identifying the proportion of families receiving services and the quality of those services by each subgroup. Such analyses can enable the state to target areas in need of improvement or intervention.
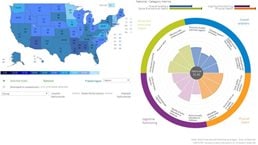
Early childhood development—a data visualization
Track funding and service journeys of children and families to identify where children are slipping through the cracks. It is important to understand why children are no longer receiving services or where state funds are inadvertently subsidizing higher-income families. Apply a “user perspective” to draw out different pathways to programs and services and (as mapped in Exhibit 3) to pinpoint common challenges, such as lack of awareness about programs or lack of coordination across programs. Ideally, the state would stitch together data from multiple sources—Medicaid, the Department of Education’s Individuals with Disabilities Education Act, and the Department of Health and Human Services—to create an objective, data-based foundation for these analyses.
Measure key elements of early childhood well-being to understand the impact of spending and services on developmental outcomes. Analyze state-level outcomes along the various dimensions of childhood well-being. These dimensions include overall enablers, such as parental support programs and developmental screening and interventions; physical health, including access to and use of quality healthcare; cognitive functioning, such as early language and numeracy exposure; and social and emotional health, such as effective child welfare programs and minimizing adverse childhood events, including abuse and neglect. Exhibit 6 provides an example of how a state might use these indicators to assess its performance and focus on areas of improvement to spend existing dollars more efficiently.

Phase 2: Strategy and planning
Prioritize individual interventions to improve outcomes on specific dimensions of overall early childhood well-being. Building off the insights generated during Phase 1, prioritize targeted interventions to address each of those state-specific areas of need. For example, if very few four-year-old children are served by state pre-K, it is important to prioritize interventions to increase pre-K access, whether by expanding facilities, recruiting and retaining talent, or reallocating funding from less-efficient interventions. Best practice dictates that the design of these targeted interventions should be evidence based—for example, when increasing access to pre-K, programs could use methods to support quality teacher-child interactions and the pre-K input shown to yield the largest improvement in pre-K outcomes.22 This focus on evidence ensures that dollars are spent only where they will generate the most positive impact for children and communities.
Develop cross-agency intervention strategies to integrate spending and services that are optimized to improve child outcomes. To ensure investments in health, education, and other social services achieve their desired effects, it is helpful to coordinate the provision of services across agencies along the social safety net. Best practices in interagency collaboration include but are not limited to the following:
- Bridge cultures across agencies. Understand missions and organizational cultures of each agency and develop consistent and mutually agreed-upon terminology, definitions, and processes.
- Develop a system to track outcomes and accountability. Define short- and long-term outcomes clearly and ensure alignment so as not to duplicate outcomes tracked across agencies. Create an interagency dashboard that tracks outcomes and access to services available to children and families across agencies.
- Clarify roles and responsibilities. Identify owners for specific services, ensure cross-agency overlap only when necessary, and minimize duplication of provisions where possible. This clarity is especially important when roles are shared.
- Coconstruct strategies and implementation plans. Ensure alignment across spending, services, and overall cross-agency operation. Include details such as an implementation road map, a stakeholder engagement plan, a measurement and evaluation plan, and a strategy for agency collaboration.
Phase 3: Implementation and scaling
Launch pilots to test new strategies on a small scale and prepare for broader rollout across the state. Select a few geographies that are high need or that have the desired environment for potential pilots. During the pilot phase, provide coaching and extra capacity to relevant stakeholders where possible to accomplish priority initiatives. Establish health and education implementation teams to accelerate execution with designated personnel to provide support and guidance on budgetary resource allocation, stakeholder engagement, measurement and evaluation, and cultural and behavioral shifts needed within state and local agencies. Share impact and results with key stakeholders to inform a revised strategy ahead of a broader rollout.
Support agencies to scale those interventions found to be most effective. Put systemwide infrastructure and supports in place to ensure success. States could first assess the capacity of other regions to implement what the pilot regions undertook. They can also develop a plan to support regions with weaker infrastructure in the early days of implementation. States could further work to create habits and routines that sustain implementation and promote continuous improvement. For example, states can track progress against each initiative’s expected trajectory and review findings through regular check-ins and reviews to solve any problems that might arise.
Despite a high per capita income, the United States scores poorly in several measures of child well-being. In fact, a 2016 UNICEF report of 41 wealthy nations places the United States tenth on education inequality, 14th on health inequality, and 30th on income inequality.23 These scores suggest a need for action and targeted improvement efforts—and each state has a unique role to play.
By laying the groundwork for success, ensuring true cross-agency interventions, and implementing and scaling effective programming, states can potentially save hundreds of billions of dollars and ensure that kids stop falling through the cracks of the health and education systems—and start growing into happy, healthy, and productive members of society.


