Despite using oxygen medically for over 100 years and WHO classifying it as an essential medicine in 2017, large population groups, especially in developing countries, do not have access to adequate supplies. WHO has consistently raised alerts about the ongoing and persistent shortages in Africa, the Middle East, and other developing regions.1 The adverse impact of the shortage is most critically felt in neonatal care, with an estimated half a million newborns around the world dying annually from oxygen shortages.
As COVID-19 patient-care protocols have evolved, medical-grade oxygen is considered essential to treatments for critically ill patients, such as invasive ventilation and low- and high-flow oxygen therapies. In regions such as Africa and the Middle East, the surge in demand for medical oxygen to treat COVID-19 exacerbates preexisting gaps in medical-oxygen supplies, leading to substantial supply shortages (Exhibit 1). Even though these regions may have lower incremental demand for oxygen to treat COVID-19 than, say, China, their lower preexisting supplies will contribute to greater shortages.2

In this article, we explore potential ways to solve the supply shortage, help countries respond to the COVID-19 pandemic, and close the structural deficiencies in oxygen supply for large population groups.
Medical-oxygen supply chain
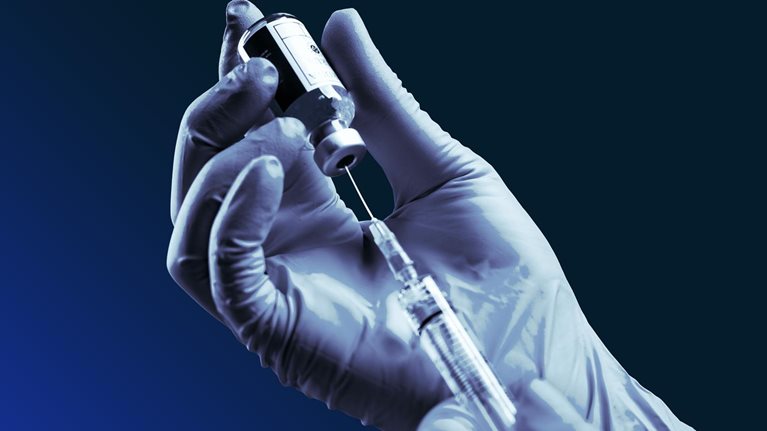
Medical oxygen is produced at plants in quantity and delivered to hospitals in bulk in liquid tanks or in smaller amounts as pressurized gas in cylinders (Exhibit 2), depending on a hospital’s specific needs and infrastructure. Liquid oxygen, once received at hospitals, is distributed to patients through an internal network of pipes. Thus, hospitals need to have the right infrastructure, including cryogenic tanks, vaporizers, and piping throughout buildings, to have liquid oxygen delivered.3 Pressurized oxygen-gas cylinders do not require internal piping systems. They can be used in hospitals without a sophisticated infrastructure and in facilities such as clinics that do not need high-volume or continuous oxygen supplies. Cylinders are also commonly used for supplemental or emergency supply in hospitals that rely primarily on liquid deliveries.

Regional disparities in medical-oxygen supply
While medical-oxygen production can be scaled to meet global demand, long-distance oxygen transportation has not been regarded as economically efficient, so favored sources are almost all local. Therefore, the primary consideration for a country’s ability to meet COVID-19-related oxygen demand adequately has been the maturity of its existing production and distribution infrastructures.
Developed regions such as the United States and Western Europe are thought to have relatively mature and sound medical-oxygen infrastructures, and incremental demand is likely to pose little threat to their supply chains. These regions generally had a sufficient supply of oxygen to meet prepandemic demand and have not experienced significant shortages during the pandemic. To provide continuous oxygen supplies, they redistributed medical oxygen from nonessential or underutilized healthcare facilities and repurposed existing nonmedical supplies. They also expanded delivery systems at healthcare facilities, such as pipeline networks and vacuum-insulated evaporators at hospitals.
On pins and needles: Will COVID-19 vaccines ‘save the world’?
However, many countries with less-developed medical-oxygen infrastructures were already presumed to be struggling with an oxygen shortage before the COVID-19 pandemic. With limited supplies, they will need to consider a multistep approach to bolster their systems.4 There are immediate, intermediate, and longer-term solutions to explore:
- Short term. A potential short-term solution for medical-oxygen shortages at hospitals is to deploy oxygen concentrators. These devices filter medical-grade oxygen from ambient air through an internal filtration system. Additionally, they are not subject to several of the supply-chain constraints of medical oxygen, such as transportation and recurring deliveries. Limited flow rates of oxygen delivery make concentrators a less-effective treatment for severe cases. They can, however, be considered for providing low-flow oxygen to less-critical patients so that higher-flow-rate supplies can be reserved for critical patients. Despite the additional costs of concentrators, including their consumables, maintenance, and power, they are regarded as a relatively quick-and-easy way to meet increased demand in regions with less-developed infrastructure. Deploying inexpensive pulse oximeters could also help ensure that oxygen therapies are targeted where they are most needed.
- Medium term. Medical oxygen accounts for approximately 3 percent of global oxygen production. So a medium-term solution could be to repurpose the oxygen produced by industries outside of healthcare, such as garment manufacturers that make oxygen for bleaching and steel manufacturers that make it for their operations. These sources could be repurposed for healthcare with the requisite quality and tracking measures. To increase capacity quickly, however, would require regulatory approval—for example, the United Nations Economic Commission for Europe’s emergency multilateral agreement extends the inspection-validity period for the vehicles and tanks used to transport medical gases.5 Also, the Indian government approved a measure allowing industrial manufacturers to produce medical oxygen. If these challenges can be met, alternate oxygen sources are potentially relatively quick ways to increase supply.
- Long term. The most likely lasting solution to the medical-oxygen shortage is to increase the capacity of existing medical-oxygen producers permanently. This can be done by investing in production equipment, such as cryogenic air separators, and by increasing the number of shifts. However, depending on the installed capacity and the availability of trained operators, this can be time consuming and capital intensive. Also, for these additional volumes to reach patients will require a higher-capacity distribution infrastructure, including traceable tanks, gas-carrier trucks, qualified distribution personnel, and optimized delivery routes.
Such interventions may not only help close the immediate COVID-19-related shortfall in medical-oxygen supply but also go a long way to eliminating the chronic undersupply of medical oxygen in those countries.
The COVID-19 crisis has brutally exposed the shortage of medical oxygen in many countries, making what was already considered a bad situation worse. If immediate actions are taken with the foresight and commitment to fix systemic deficiencies, investments in medical oxygen to treat COVID-19 have the potential to help reduce the global supply shortage for good.