The COVID-19 pandemic has emerged as one of the most significant humanitarian challenges in recent history, and testing is seen as one of the main components of efforts to contain the virus and mitigate its impact.
There are two main testing technologies: molecular assays, which identify viral genetic material and signal the presence of a viral infection, and immunoassays, which identify antigens or antibodies. While both types of tests are considered important in developing a successful COVID-19-response strategy, this article focuses on molecular-assay testing, regarded as the confirmatory test for detecting active infections—and specifically on laboratory-based molecular-assay tests as opposed to point-of-care tests. While the latter can play an important role in a testing strategy, they are deployed on a much smaller scale (see sidebar, “Testing technologies”).
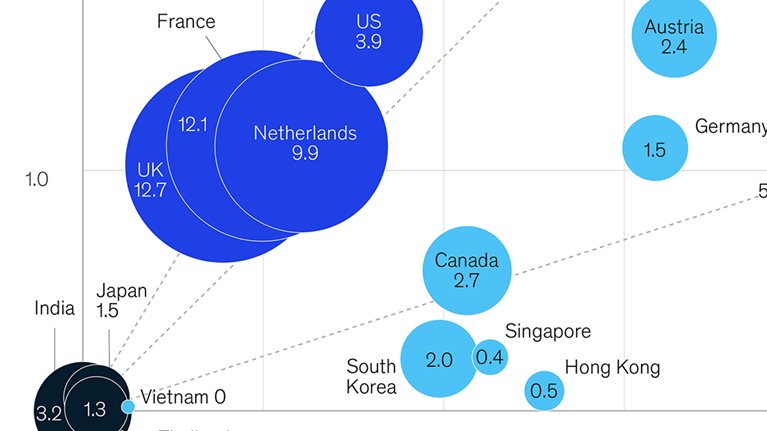
Many regions around the world are experiencing a shortage of laboratory-based molecular-assay tests. In the United States, for example, testing capacity stands at between three and three-and-a-half million tests a week, well below even some of the most conservative estimates of the number required.1 The estimated number needed ranges from six million tests a week (if the economy is to be partially reopened) to 20 million a day, representing 6 percent of the population each day (if it is to be fully reopened while still controlling outbreaks).2 To put that into perspective, the current global capacity for molecular tests within laboratories is estimated to be around 14 million to 16 million tests a week, with the number of tests actually conducted being less than 10 million per week (Exhibit 1).3

Increasing the supply of tests—as well as ensuring that they reach those who need them—is therefore crucial. Even as disease-prevalence rates fall and economies reopen, identifying those who are infected will likely remain a priority—both to treat and isolate them and to further epidemiological knowledge of the disease. This article examines where constraints in the process for delivering tests currently lie to help identify how efforts might be directed to ease them.
Where constraints lie
There are five main activities in the process for delivering laboratory-based molecular-assay tests: sample collection, logistics, test execution, data management, and testing-capacity management (Exhibit 2). (Data management is not examined in this article.) All activities need to be executed harmoniously to maximize supply in a complex testing ecosystem, but bottlenecks can occur at each point.

Sample collection
Sample collection is required for all diagnostic testing. A shortage of the supplies needed to collect samples (such as swabs and viral-transport mediums) and a limited number of testing sites have sometimes led to long waiting times for a COVID-19 test and to key segments of the population (such as healthcare workers) going untested.
Progress on addressing some of these issues has been made. To increase the supply of swabs, traditional manufacturers have increased capacity, new manufacturers have been approved, and some manufacturers are using 3-D printing. Some health authorities have approved alternative transport mediums (such as saline) and different types of samples (such as saliva and lower-respiratory-tract samples). Studies indicate that the test results from such alternatives could be as accurate as those taken from swabs.4
To collect more samples, countries have also expanded testing sites by establishing drive- and walk-through testing centers. Such centers help reduce not only waiting times but also the risk of contagion to healthcare providers and others. At-home sample-collection methods are also emerging as relatively safe options and have been validated by several countries.5
Logistics
Logistics companies play a crucial role at two points in the testing supply chain: the shipment of components from sources around the world to testing laboratories and the transportation of samples from collection points to laboratories. Neither issue has proved to be as significant a constraint on testing as the other issues highlighted in this article. They could, however, become more problematic as countries (particularly those with emerging economies) expand testing, so both issues should be monitored closely.
Test execution
Two main challenges have led to a limited capacity to execute tests: a shortage of the laboratory equipment and trained personnel needed to run tests and a shortage of the necessary reagents, which are often packaged as kits (testing kits and RNA-extraction kits, for example).
Building and installing new equipment takes time—between 20 and 30 days for an order of high-throughput equipment to be delivered, for instance, and at least three to five days for it to be installed, calibrated, and validated for diagnostic testing.6 Newly installed equipment also requires more trained personnel to operate it. Moreover, financial constraints in many countries—government funding for public health laboratories, for example—can make it hard to build additional capacity.
Executing a test requires some 20 different reagents, consumables, and other pieces of equipment. Of those materials, major shortages have been reported in RNA-extraction kits and certain reagents, including enzymes and primers.7 The global manufacturing capacity for molecular-assay tests is estimated to be between 37 million and 38 million tests a week, given current availability of the various test components, with RNA-extraction kits being the bottleneck to higher capacity (Exhibit 3).8 That compares with fewer than 10 million tests a week being conducted around the world, according to our research.

There are two potential explanations for the gap. First, a significant quantity of the reagents being manufactured are those that run on open systems—that is, less integrated systems that can run a wider range of test methods. Such reagents cannot be used with the high-throughput machines that tend to be used in developed countries and are closed systems requiring cartridges loaded with proprietary reagents manufactured by the OEM. Second, as Exhibit 3 shows, most of the available manufacturing capacity is based in China, potentially making access to it more difficult, given validation and export considerations.
Testing-capacity management
In some countries, matching supply with demand has been a bottleneck, leaving available laboratory-testing capacity underutilized. Laboratories in various locations around the United States, for example, have reported unused capacity to conduct more tests, even as patients and healthcare workers report difficulty in securing tests.9 A similar situation has arisen in the United Kingdom, where the number of completed tests has often lagged behind reported capacity.10
The same is true of supplies of reagents, test kits, and other consumables. In April 2020, Brazil reported that seven laboratories cleared by health regulators were unable to process tests because they did not have the reagents, even though they were available on the market.11 Lack of coordination, experienced in locations around the world, has often led to unnecessary competition for supplies among regions and even among hospitals within a single region.12
Bridging the supply–demand gap
The previously described constraints in the testing process that have emerged to date suggest what might be done to bridge the supply–demand gap. Some of the measures will bring about incremental improvements and others a step change, but both will likely be required to bridge the gap. Measures require different level of investments. And some are short-term measures capable of delivering results in as little as three months, while others will take longer—possibly up to a year or longer.
Short-term measures
Three measures could help maximize the utilization of existing resources in as few as three months.
1. Establish visibility into testing capacity. A clear view of the unused testing capacity available is crucial if it is not to go to waste. Here, the establishment of information nerve centers that collect data on local capacity then match it with demand on a daily basis could help. As more capacity comes on stream, a nerve center’s overview could also help health authorities expand testing quickly—for example, offering tests not only to healthcare workers and those in hospital but also to vulnerable members of the community. Nerve centers could also act as a repositories for critical data on the inventory levels of consumables and testing reagents and on potential suppliers, helping governments and healthcare providers plan ahead and prevent shortages.
2. Maximize existing laboratory capacity. Local laboratories may not be fully utilizing installed equipment for a number of reasons, ranging from suboptimized workflows to lack of trained personnel. Unlocking all available capacity starts by compiling a full inventory of the installed equipment base, distinguishing between open and closed systems, then calculating the maximum theoretical laboratory capacity, given the installed base. That allows companies to locate and address bottlenecks, be it by establishing new workflows, hiring additional personnel, or finding alternative suppliers of reagents if open-source systems are used. Universities and major diagnostic manufacturers could perhaps partner with local laboratories to help with some of those issues—providing open-system equipment they have in their own research facilities, reagents, and trained personnel, for example.
3. Establish new laboratory capacity. Laboratory capacity can be raised by increasing the equipment footprint in existing laboratories and by establishing new, high-capacity laboratories. Collaboration among governments, public-health organizations, equipment manufacturers, and private laboratories can accelerate such efforts. Novacyt, a UK and French diagnostics company, has collaborated with AstraZeneca, GlaxoSmithKline, and the University of Cambridge to increase testing capacity in the United Kingdom, for example.13
As shortages of testing kits can cause bottlenecks within laboratories, an important consideration when installing new capacity is which type of equipment to install: open systems, which can run a wider range of test methods, or closed systems, which require proprietary reagents manufactured by OEMs. The choice could have a significant impact on future testing capacity, as reagents for open systems are manufactured by considerably more suppliers.
If open systems are chosen, health authorities may still wish to consider evaluating and validating new sources of supply to mitigate the risk of future shortages. Establishing a centralized repository that holds information on the performance of various kits and their components could help speed the validation and approval processes. And prioritizing the validation of suppliers with high capacity would likely grant faster access to additional manufacturing capacity.
Medium-term measures
Two measures could boost capacity in the medium term (that is, between three months and a year or longer).
1. Scale up production of closed-system cartridges and proprietary reagents. One of the main reasons that laboratories using closed-system equipment have been underutilized during the current pandemic is a shortage of the OEMs’ cartridges loaded with proprietary reagents. To utilize these systems closer to their theoretical maximum capacity, OEMs will need to ramp up production volumes, though doing so is a tough decision to make, given the costs involved and the risks when long-term demand is uncertain.
2. Explore alternative testing protocols and ‘curve shifting’ technologies. As previously mentioned, alternative protocols for sample collection and testing can help increase testing capacity and alleviate shortages of particular components, and some of these protocols have already been validated by various authorities. In addition, sample pooling can be used to decrease the quantities of reagents needed.14
New and potentially curve-shifting testing technologies can also be explored. For instance, large-scale next-generation sequencing can potentially run up to 100,000 pooled samples in a single machine in eight to 12 hours. That could increase testing capacity by an order of magnitude, assuming the availability of reagents, instruments, heating capacity, and trained personnel to preprocess samples. Such technologies are still in the research phase, but there may be an opportunity to validate and scale them rapidly once real-world evidence of their performance is available.
New techniques could also facilitate more at-home tests. For instance, companies such as Caspr Biotech, Mammoth Biosciences, and Sherlock Biosciences are developing at-home, CRISPR-based tests that utilize reagents different from those in traditional molecular-assay tests.15
Impressive efforts by public and private bodies alike have seen the rapid escalation of the capacity of laboratory-based molecular-assay testing in some regions, but there are opportunities around the world to increase it further. Focusing efforts on a select set of high-impact measures, as described in this article, could make an important difference. As immunoassay testing begins to play a larger role in local and global responses to the COVID-19 pandemic, similar analysis and focus will be needed to increase testing capacity. Without doubt, increasing testing capacity is a daunting challenge, but it is one that needs to be met to help ensure more reliable virus control and more sustainable economic recovery.