On the surface, Japan’s health care system seems robust. The country’s National Health Insurance (NHI) provides for universal access. Japan’s citizens are historically among the world’s healthiest, living longer than those of any other country. Infant mortality rates are low, and Japan scores well on public-health metrics while consistently spending less on health care than most other developed countries do.
Yet appearances can deceive. Our research indicates that Japan’s health care system, like those in many other countries, has come under severe stress and that its sustainability is in question.1 The conspicuous absence of a way to allocate medical resources—starting with doctors—makes it harder and harder for patients to get the care they need, when and where they need it. A vivid example: Japan’s emergency rooms, which every year turn away tens of thousands who need care. Furthermore, the quality of care varies markedly, and many cost-control measures implemented have actually damaged the system’s cost effectiveness.
Meanwhile, demand for care keeps rising. For a long time, demand was naturally dampened by the good health of Japan’s population—partly a result of factors outside the system’s control, such as the country’s traditionally healthy diet. Yet rates of obesity and diabetes are increasing as people eat more Western food, and the system is being further strained by a rapidly aging population: already 21 percent of Japan’s citizens are 65 or older, and by 2050 almost 40 percent may be in that age group. Furthermore, advances in treatment are increasing the cost of care, and the system’s funding mechanisms just cannot cope.
So Japan must act quickly to ensure that its health care system can be sustained. It must close the funding gap before it becomes irreconcilable, establish greater control over supply of services and demand for health care, and change incentives to ensure that they promote high-quality, cost-effective treatment. Many of the measures needed address a number of problems simultaneously and may prove instructive for other countries.
Japan’s challenges
Underlying the challenges facing Japan are several unique features of its health care system, which provides universal coverage through a network of more than 4,000 public and private payers. All residents must have health insurance, which covers a wide array of services, including many that most other health systems don’t (for example, some treatments, such as medicines for colds, that are not medically necessary).
The system imposes virtually no controls over access to treatment. There is no gatekeeper: patients are free to consult any provider—primary care or specialist—at any time, without proof of medical necessity and with full insurance coverage. Similarly, Japan places few controls over the supply of care. Physicians may practice wherever they choose, in any area of medicine, and are reimbursed on a fee-for-service basis. There is also no central control over the country’s hospitals, which are mostly privately owned. These characteristics are important reasons for Japan’s difficulty in funding its system, keeping supply and demand in check, and providing quality care.
Funding the system
Japan’s health care system is becoming more expensive. In 2005 (the most recent year with available comprehensive data), the cost of the NHI plan was 33.1 trillion yen ($333.8 billion at March 2009 rates), or 6.6 percent of GDP.2 By 2020, our research indicates, that could rise to 62.3 trillion yen, almost 10.0 percent of GDP, and by 2035 it could reach 93.6 trillion yen, 13.5 percent of GDP. True, the current cost—low by international standards—is projected to grow only to levels that the United States and some European countries have already reached. Yet funding the system is nonetheless a challenge, for Japan has by far the highest debt burden in the OECD,3 a rapidly aging population, and a stagnating economy.
Why costs are rising. Four factors account for Japan’s projected rise in health care spending (Exhibit 1). Advances in medical technology—new treatments, procedures, and products—account for 40 percent of the increase. The country’s growing wealth, which encourages people to seek more care, will be responsible for an additional 26 percent, the aging of the population for 18 percent. The remaining 16 percent will result from the shifting treatment patterns required by changes in the prevalence of different diseases.
Four underlying causes
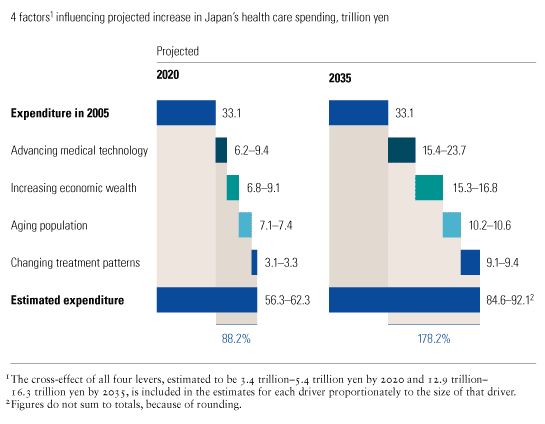
Japan can do little to influence these factors; for example, it cannot prevent the population’s aging. Delays in the introduction of new technologies would be both medically unwise and politically unpopular. Yet unless the current financing mechanisms change, the system will generate no more than 43.1 trillion yen in revenue by 2020 and 49.4 trillion yen by 2035, leaving a funding gap of some 19.2 trillion yen in 2020 and of 44.2 trillion yen by 2035.
Compounding matters is Japan’s lack of central control over the allocation of medical resources. No agency or institution establishes clear targets for providers, and no mechanisms force them to take a more coordinated approach to service delivery. Just as no central authority has jurisdiction over hospital openings, expansions, and closings, no central agency oversees the purchase of very expensive medical equipment. As a result, Japan has three to four times more CT, MRI, and PET scanners per capita than other developed countries do. Most of these machines are woefully underutilized.
No easy answers. Japan must find ways to increase the system’s funding, cost efficiency, or both. Traditionally, the country has relied on insurance premiums, copayments, and government subsidies to finance health care, while it has controlled spending by repeatedly cutting fees paid to physicians and hospitals and prices paid for drugs and equipment. That has enabled Japan to hold growth in health care spending to less than 2 percent annually, far below that of its Western peers. At some point, however, increasing the burden of these funding mechanisms will place too much strain on Japan’s economy.
If, for example, Japan increased government subsidies to cover the projected growth in health care spending by raising the consumption tax (which is currently under discussion), it would need to raise the tax to 13 percent by 2035. But the country went into a deep recession in 1997, when the consumption tax went up to the current 5 percent, from 3 percent. Similarly, a large spike in insurance premiums would increase Japan’s labor costs and damage its competitive position. Markedly higher copayment rates would undermine the concept of health insurance, as rates today are already at 30 percent.
Even if Japan increased all three funding mechanisms to cover the system’s costs, it risks damaging its economy. If copayment rates increased to 40 percent, premiums would still have to rise by 8 to 13 percentage points and the consumption tax by up to 6 percentage points (Exhibit 2). In the current economic climate, these choices are not attractive. Nevertheless, the country will have to resort to some combination of increases to cover the rise in health care spending.
No cheap fix
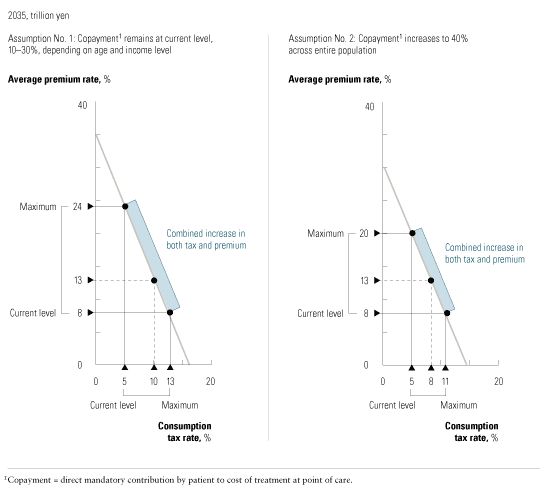
Japan has repeatedly cut the fees it pays to physicians and hospitals and the prices it pays for drugs and equipment. This approach, however, is unsustainable. Fee cuts do little to lower the demand for health care, and prices can fall only so far before products become unavailable and the quality of care suffers. In addition, the country typically applies fee cuts across the board—a politically expedient approach that fails to account for the relative value of services delivered, so there is no way to reward best practices or to discourage inefficient or poor-quality care.
Mismatched supply and demand
Japan combines an excess supply of some health resources with massive overutilization—and shortages—of others.4 On average, the Japanese see physicians almost 14 times a year, three times the number of visits in other developed countries. The introduction of copayments and subsequent rate increases have done little to reduce the number of consultations; what’s more, the average length of a hospital stay is two to three times as long in Japan as in other developed countries. In neither case can demographics, the severity of illnesses, or other medical factors explain the difference.
The country’s health system inadvertently promotes overutilization in several ways. For starters, there is evidence that physicians and hospitals compensate for reduced reimbursement rates by providing more services, which they can do because the fee-for-service system doesn’t limit the supply of care comprehensively. Japan’s physicians, for example, conduct almost three times as many consultations a year as their colleagues in other developed countries do (Exhibit 3).
Overutilization
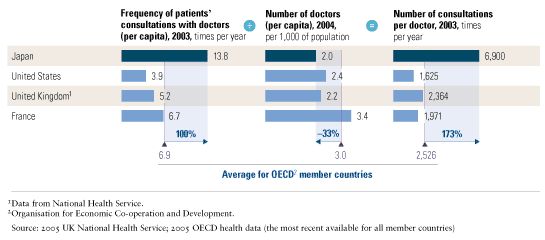
Furthermore, Japan’s physicians can bill separately for each service—for example, examining a patient, writing a prescription, and filling it.5 No surprise, therefore, that Japanese patients take markedly more prescription drugs than their peers in other developed countries. The system also rewards hospitals for serving larger numbers of patients and for prolonged lengths of stay, since no strict system controls these costs.6
Nevertheless, most Japanese hospitals run at a loss, a problem often blamed on the system’s low reimbursement rates, which are indeed a factor. Another is the health system’s fragmentation: the country has too many hospitals—mostly small, subscale ones. On a per capita basis, Japan has two times more hospitals and inpatients and three times more hospital beds than most other developed countries. Our analyses suggest a direct relationship between the number of beds and the average length of stay: the more free beds a hospital has, the longer patients remain in them.
Although Japanese hospitals have too many beds, they have too few specialists. One reason is the absence in Japan of planning or control over the entry of doctors into postgraduate training programs and specialties or the allocation of doctors among regions. Another is the fact that the poor economics of hospitals makes the salaries of their specialists significantly lower than those of specialists at private clinics, so few physicians remain in hospital practice for the remainder of their working lives. High consultation rates and prolonged lengths of stay exacerbate the shortage of hospital specialists by forcing them to see high volumes of patients, many of whom do not really require specialist care. As a result, too few specialists are available for patients who really do require their services, especially in emergency rooms. Japan has an ER crisis not because of the large number of patients seeking or needing emergency care but because of the shortage of specialists available to work in emergency rooms.
Quality of care
Given the health system’s lack of controls over physicians and hospitals, it isn’t surprising that the quality of care varies markedly. Among patients with stomach cancer (the most common form of cancer in Japan), the five-year survival rate is 25 percent lower in Kure than in Tokyo, for example. Four factors help explain this variability.
First, Japan’s hospital network is fragmented. Research has repeatedly shown that outcomes are better when the centers and physicians responsible for procedures undertake large numbers of them. Because Japan has so many hospitals, few can achieve the necessary scale. In a year, the average Japanese hospital performs only 107 percutaneous coronary interventions (PCI), the procedure that opens up blocked arteries, for example. This is half the volume that the American Heart Association and the American College of Cardiology recommend for good outcomes. (In other developed countries, the average number of PCIs per hospital ranges from 381 to 775.) The small scale of most Japanese hospitals also means that they lack intensive-care and other specialized units. Few Japanese hospitals have oncology units, for instance; instead, a variety of different departments in each hospital delivers care for cancer.7
Second, Japan’s accreditation standards are weak. Doctors receive their medical licenses for life, with no requirement for renewal or recertification. No central agency oversees the quality of these physicians’ training or the criteria for board certification in specialties, and in most cases the criteria are much less stringent than they are in other developed countries.
Third, the system lacks incentives to improve the quality of care. Japan has few arrangements for evaluating the performance of hospitals; for example, it doesn’t systematically collect treatment or outcome data and therefore has no means of implementing mechanisms promoting best-practice care, such as pay-for-performance programs. Similarly, it has no way to enable hospitals or physicians to compare outcomes or for patients to compare providers when deciding where to seek treatment.
Finally, the quality of care suffers from delays in the introduction of new treatments. Specialists are too overworked to participate easily in clinical trials or otherwise investigate new therapies. And because the country has so few controls over hospitals, it has no mechanism requiring them to adopt improvements in care. Furthermore, the agency responsible for approving new drugs and devices is understaffed, which often delays the introduction or wide adoption of new treatments for several years after they are approved and adopted in the United States and Western Europe.
The way forward
There are no easy answers for restoring the vitality of an ailing health care system. Political realities frequently stymie reform, while the life-and-death nature of medical care makes it difficult to justify hard-headed economic decision making. If Japan, with all its unique features, can make progress in tackling its problems—funding, supply, demand, and quality—then other nations seeking to overhaul their health systems should pay careful attention both to the substance of its reforms and to the way it navigates the treacherous waters ahead.
The substance of reform
To close the system’s funding gap, Japan must consider novel approaches. One possibility: allowing payers to demand outcome data from providers and to adopt reimbursement formulas encouraging cost effectiveness and better care. Another option is a voluntary-payment scheme, so that individuals could influence the amount they spend on health care by making discretionary out-of-pocket payments or up-front payments through insurance policies. Such schemes, adopted in Germany and Switzerland, capitalize on the fact some people are willing to pay significantly more for medical services, usually for extras beyond basic coverage. Our research shows that augmenting Japan’s current system with voluntary payments could reduce the funding gap by as much as 25 percent as of 2035.
Japan could increase its power over the supply of health services in several ways. Incentives and controls can reduce the number of hospitals and hospital beds. One example: offering financial incentives or penalties to encourage hospitals (especially subscale institutions) to merge or to abandon acute care and instead become long-term, rehabilitative, or palliative-care providers. Similarly, monetary incentives and volume targets could encourage greater specialization to reduce the number of high-risk procedures undertaken at low-volume centers. The country should also consider moving away from reimbursing primary care through uncontrolled fee-for-service payments. Capitation, for example, gives physicians a flat amount for each patient in their practice.
Finally, the adoption of a standardized national system for training and accrediting specialists would be a critically important way to address Japan’s shortage of them. Exerting greater control over the entry of physicians into each specialty and their allocation among regions, both for training and full-time practice, would of course raise the level of state intervention above its historical norm.
The demand side of Japan’s health system invites greater intervention as well. Important first steps would include more strictly limiting services covered in order to eliminate medically unnecessary ones, as well as mandating flat fees based on patients’ diagnoses to reduce the length of hospital stays. To encourage the participation of payers, the system could allow them to compete with each other, which would provide an incentive to develop deep expertise in particular procedures and allow payers to benefit financially from reform. They could receive authority to adjust reimbursement formulas and to refuse payment for services that are medically unnecessary or don’t meet a cost effectiveness threshold.
Another piece of the puzzle is to make practicing in hospitals more attractive for physicians; higher payment and compensation levels, especially for ER services, must figure in any solution. In addition, Japan’s health system probably needs two independent regulatory bodies: one to oversee hospitals and require them to report regularly on treatments delivered and outcomes achieved, the other to oversee training programs for physicians and raise accreditation standards.
A process for reform
Awareness of the health system’s problems runs high in Japan, but there’s little consensus about what to do or how to get started. A productive first step would be to ask leading physicians to undertake a comprehensive, well-funded national review of the system in order to set clear targets. Such an approach enabled the United Kingdom’s National Health Service to make the transition from talking about the problem of long wait times to developing concrete actions to reduce them.
Next, reformers should identify and implement quick wins—short-term operational improvements that produce immediate, demonstrable benefits—to build support for the overall reform effort, especially longer-term or politically contentious changes. A few success stories have already surfaced: several regions have markedly reduced ER utilization, for example, through relatively simple measures, such as a telephone consultation service combined with a public education campaign. Reform can take place in stages; it doesn’t have to be an all-or-nothing affair.
Nor must it take place all at once. Indeed, shifting expectations away from quick fixes, such as across-the-board fees for physicians or lower prices for pharmaceuticals, will be an important part of the reform process. Significant departures from current practice would be needed to implement alternatives such as pay-for-performance programs rewarding physicians for high-quality care and penalizing them for inadequate or inefficient care, or the use of generic drugs through forced substitution or generic reference pricing, which would free up funds for new, innovative, and often more expensive treatments.8 These measures will call for a significant communications effort to explain the reforms and show why they are needed.
Japan confronts a familiar and unpleasant malady: the inability to provide citizens with affordable, high-quality health care. By making the right choices, it can control health system costs without compromising access or quality—and serve as a role model for other countries.