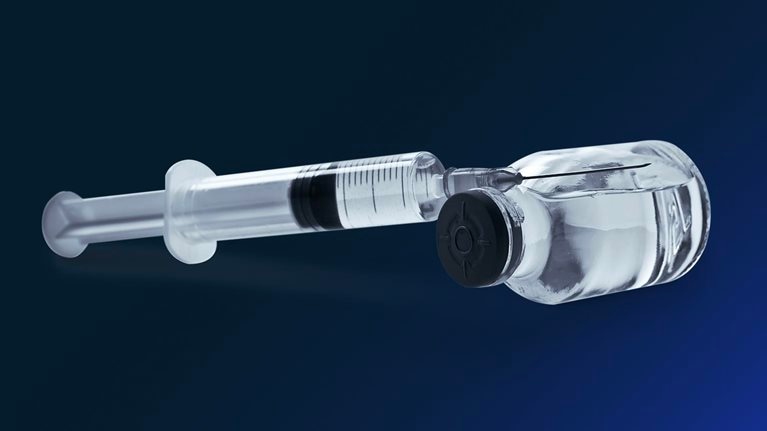
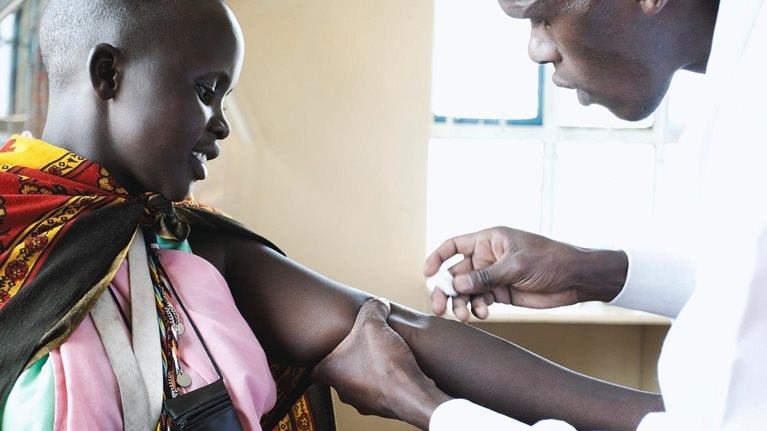
As policymakers vaccinate their populations against an ever-changing COVID-19, they’re discovering numerous challenges along the way. In this episode of The McKinsey Podcast, McKinsey partners Lieven Van der Veken and Tania Zulu Holt share insights on progress and lessons learned so far, and how to help get the vaccine distributed as quickly and safely as possible. An edited transcript of their conversation follows.
Diane Brady: Hello and welcome to The McKinsey Podcast. I’m Diane Brady. The COVID-19 vaccines are here, and that has been creating a lot of hope and challenges for how to make these vaccines available on an unprecedented scale. Joining me today to talk about how we can achieve this, and the lessons learned so far, are two McKinsey partners who’ve been doing a lot of work in this area. Lieven Van der Veken is a senior partner in McKinsey’s Geneva office. A doctor by training, he leads our social sector and our public health work in Europe. Lieven, welcome.
Lieven Van der Veken: Good to be here.
Diane Brady: And Tania Zulu Holt is a healthcare economist and partner in the London office, where she works with donor institutions globally, including on vaccine delivery. Tania, welcome.
Tania Zulu Holt: Thank you, Diane.
Diane Brady: So, Lieven, where are we at this stage in the distribution?
Lieven Van der Veken: We have to start by recognizing that there are a large number of countries that have not started vaccinations yet. Those that have started are in very different stages of the rollout. Having said that, it is clear that all countries go through roughly four phases as their systems are scaling, as their supply scales, and as their demand evolves over time.
They go from an initial phase, which is all about getting early-access authorization and then early supplies, which are often very limited, to a second phase, when the delivery systems are scaling—often with a little bit of a time lag behind supplies.
Then there’s the phase when the systems to vaccinate are up and running and new innovations such as vaccination centers are brought online, but the supply starts to fall short again. There’s a final phase when there is a system that works very well and can scale. The supply is getting to levels that are more significant. That’s when demand starts to be an issue. There is one country today, Israel, that is in that scenario.
Diane Brady: Tania, I’ll go to you in terms of the challenges now with regard to supply.
Tania Zulu Holt: One of the questions that many people are asking themselves is whether there’ll be enough vaccines for the world. There are many unknowns. On the one hand, there’s a diverse group of authorized, but also pipeline, vaccine products from producers from all over the world. On the other hand, there are also unknowns about the manufacturing-capacity scale-up and scale-out.
If we do take a look at just the publicly announced capacity of all the manufacturers that have a vaccine authorized in at least one country, we’re actually looking at enough manufacturing capacity to cover roughly 85 percent of the world’s population. If we are adding some of the vaccines that are still in late-stage development, we’ll probably get up toward 100 percent of the global population being able to have vaccines by the end of 2021. Of course, that's the total that will be manufactured. A lot else needs to happen for these vaccines to reach that percentage of the population.
Diane Brady: Here in the US, there’s been a strain of euphoria that the pandemic is almost over. Yet at the same time, Lieven, I keep hearing about these new variants of the virus. How does that change the scenario planning for this?
‘Nobody is safe until everybody is safe’
Lieven Van der Veken: First of all, the arrival of new variants shouldn’t surprise anybody. The viral strains have been evolving all along. Having said that, it is a very important and very urgent reminder that nobody is safe until everybody is safe. And that means we need to vaccinate everyone.
Even if a country today may be protected from the devastating effects of the COVID-19 pandemic raging through a population by vaccination, unless everybody in the world actually achieves a sufficient level of protection, new variants can keep emerging. There are scenarios when the vaccines that we currently have do not confer protection against these variants.
Tania Zulu Holt: I want to put the numbers I mentioned before into perspective. The truth is that the supply picture is quite nuanced. We do know that most of the capacity has currently been contracted and reserved by a number of the high-income countries. That means that there is a significant amount of the low- and middle-income countries that have not yet received vaccines or have only received very few doses. While we, on an aggregate, might have sufficient supplies, on a country and on a per capita basis, the rollout is much more nuanced.
Diane Brady: Lieven, what are some of the lessons that we’ve learned over the past few months?
Lieven Van der Veken: First, we have to recognize that the scale-up, even though it has felt slow and painful in many settings, is of an unprecedented nature. Even those countries that may have started out of the gates a bit slower—based on certain strategic choices or certain operational challenges—most of them have actually caught up with the supply that’s available to them. That’s an incredible achievement and the result of tens and hundreds of thousands of people working tirelessly day and night to deliver on this third major challenge of the vaccine campaign: the delivery. There’s the discovery, the manufacturing scale-up, and the delivery.
As we look back, we should not forget to celebrate that the development of the vaccine has come with unprecedented speed. Never before has a vaccine been developed with this speed. Never before have we had five or six candidates that actually have been approved in countries across the world. (That number has since risen to ten.) Never before have we actually seen such a manufacturing scale-up and scale-out with collaborations across the industry, collaborations across the globe. So there’s a lot to celebrate.
Having said that, we also have learned to appreciate how fragile all of that progress is, how important it is to continue to innovate the vaccine candidates in light of new variants, how fragile the global manufacturing networks really are. If we no longer ship the right supplies and the right equipment across the world, then plants could actually come to a halt.
We have learned how fragile the delivery scale-up is in cases where communications are falling short and populations lose their trust in one or multiple of the vaccine candidates. So a lot to celebrate—unprecedented speed, unprecedented scale—but also a lot of examples of the fragility of the progress we achieved to date.
Diane Brady: Tania, you’ve done a lot of work in the past around public trust. How are we doing on that front in terms of people trusting the efficacy of the vaccine and feeling that they want to get it?
Tania Zulu Holt: So as the vaccine has been introduced in countries, what we’ve typically seen is that the willingness to take the vaccine has increased. There are a couple of outliers in some of the Asian countries. In general, it is pointing in the right direction. Of course, with vaccine hesitancy, one element is about how the average, general population is thinking. Typically, there are subpopulation groups where we see patterns of much lower demand.
That’s certainly something that we need to watch very carefully in different countries. There are already some concerning signs in certain countries around some of those subpopulations where we’re seeing higher rejection rates.
Would you like to learn more about our Public & Social Sector Practice?
The 6A framework for vaccines
Diane Brady: Lieven, there are so many factors that are swirling around with the decision making on this. Can you tell us about the “6As,” and what that does for framing the discussion? That’s “available, administrable, accessible, acceptable, affordable, and accountable.”
Lieven Van der Veken: We’ve spent a lot of time thinking about the 60, 70 elements that one needs to get right. And one needs to plan for those in parallel. First of all, you need to have the vaccines available, right? The vaccine needs to be approved by the regulators. It needs to be there with the right supply, which includes increasing manufacturing, the sourcing of the needles. It is a complex effort in its own right: the vaccine and everything else you need for the vaccination.
The second step is “administrable.” You need to be able to actually identify the patients. You need to have the vaccination centers up and running, if that’s what you’re going to use, or have your healthcare workers trained.
Third, the vaccine does need to be accessible. It needs to be in the right place at the right time. Some of these vaccines actually have five doses in one vial. That means you need to be able to have the right strategy and the right logistics to have those five vaccinations lined up in the course of a couple of hours. How do you do that?
Fourth, it needs to be acceptable. The population needs to be ready. Your healthcare workforce needs to be trained. People need to be ready to actually receive the vaccination with excitement.
Fifth, “affordable.” It is important that there are no barriers in affordability to ensure equitable access to the vaccine. And last, what we’d call “accountable,” which is a fairly broad bucket.
Diane Brady: You both come at this from a different prism: you as a doctor, Lieven. Tania, you as an economist. Tania, you have a lot of experience in this area. Are there lessons that we can draw from previous situations with regard to administering vaccines? How do you make it acceptable to everybody?
Tania Zulu Holt: This is an incredibly important topic that has been discussed for many years. And we can go back in the US, all the way to the 1950s when the polio vaccination campaign was under way. At the time, you had Elvis Presley literally going on national TV in order to motivate some people.
Diane Brady: We need an Elvis.
Tania Zulu Holt: Exactly. It’s also important that the communication is really a two-way process. It needs to be equal listening and telling at the same time. Also, we know that knowledge is important, but it’s not sufficient. We’ll need to understand different microsegments of the population to truly see what is driving the behaviors and what will ultimately drive people’s choices. We’ll need to really use all the various communication tools that are available to us: everything from the more classic public-health campaigns to using social media and other tools that are available to us now.
Lieven Van der Veken: The initial months of vaccine rollout have reinforced how critically important communication and engagement is—communication, first of all, between all of those involved and their response in the vaccination scale-up. We have unfortunately seen quite a few instances where different parts of the system that are trying to drive the vaccination are pointing fingers at each other, are not necessarily always putting the system and the acceleration first. It’s understandable because of the pressure, but it actually slows down the vaccination.
The second challenge that we’ve seen is communication within the broader set of stakeholders. Communication with healthcare professionals, communication with influencers, communication with the media, when it’s so important that there continues to be a dialogue of trust, where everybody can get access to transparent data, can get access to the right information.
Third, communication with the broader public. And there are not that many environments today where governments or health authorities actually have direct access or a trusted base channel to engage with populations. And we see when there is a certain narrative developing in a country that needs to be engaged with, these governments struggle with that.
We would continue to urge everybody involved in scaling the vaccine delivery to invest heavily in the communication with the people who plan and who structure the delivery—and with the broader stakeholder landscaping through the healthcare delivery colleagues, and then with the broader population at large. That is going to be so important in bringing this journey home.
Tania Zulu Holt: Yes. Absolutely. And not only have the lessons been taken to heart, but I think the systems are really realizing that it’s an ongoing exercise. These campaigns will be in many countries going on for the whole of 2021, and in some countries likely into 2022.
And the situation continues to change. You’re never done with the 6As. You constantly need to redo your plans every time there is a new development. And I think we should continue to expect that there are developments, whether those are new variants or whether those are new demand patterns or new vaccines that are being authorized and coming in. The systems will continue to go through updating their plans using the equivalent of a 6A framework.
Lieven Van der Veken: So the one thing that is happening today the same way it always has in these moments of crisis and epidemic or pandemic outbreaks is that there is very little time available to look around the corner. And so of course nobody has a crystal ball. But there are a number of scenarios that one can already imagine today that may have major implications for tomorrow.
For example, it’s possible that in a couple of months we’ll not just be talking about managing a supply chain of two or three different vaccines in a given community, but also actually managing two or three different vaccines, maybe four or five, with a subset of those actually being better suited for certain variants.
How do you think about that? What is your vaccination strategy in that environment? But also, logistically, how do you keep track? And how do you actually optimize and adjust your supply chain, your communication activities, your data gathering to significantly increase the complexity of the available vaccines that you are using in the context of some of these variant vaccines?
That is a scenario which is actually not unlikely, given what we know today. But it is a scenario for which not all systems actually have the bandwidth today to start planning.
Diane Brady: Lieven raises a good point, Tania. It would seem that you’d have to have a very sophisticated degree of data analytics and technology in place to really manage this rollout. How is this happening in economies that may not be at that point?
Tania Zulu Holt: I think what’s interesting around some of the low- and middle-income countries is, unlike some of the high-income countries that historically had strong flu-vaccination programs, that they haven’t experienced reaching the adult population. And many of the low- and middle-income countries have experienced it predominantly with the children immunization programs.
So you can say on one hand, these countries actually have a relatively strong starting point with some healthcare infrastructure in terms of cold chain and people who have experience with vaccination and so forth. But, of course, they don’t have the experience as such reaching the adult population.
And second, in some of the low- and middle-income countries, that’s also where today we have most of the vaccine-preventable death, meaning that many of those countries are not sufficiently reaching the population with their children immunization programs.
And so we get to a point where these countries need to scale up beyond the first 3 percent, which is typical, healthcare workers and the most vulnerable population of people within the urban centers. And I think we should expect that these countries are going to have some scale-up challenges going to the rural populations and are going to reach beyond the first 3 percent to 20 percent and so forth.
And those advances relate to having sufficient cold-chain equipment, making sure that they train enough healthcare workers, and having the required data systems so that they can report on a live basis the different vaccinations. You have to be able to know which patients got what vaccine, so then people come back for the second dose that some of the vaccines will require.
Then we make sure that person gets the same vaccine for the second dose. And they are called back into the system in a timely manner. These are of course all things that are in high-income countries to a large extent and are being done and managed with fairly sophisticated data and information systems.
We are seeing that low- and middle-income countries are rapidly investing and investing into those systems and scaling them up. And hopefully they’ll do that in a timely manner, not just for the impact of this current pandemic, but also for the general immunization systems in these countries that are still at times lagging behind from a coverage perspective.
Subscribe to the McKinsey Talks Talent podcast
Diane Brady: One of the challenges it seems in this campaign is that we have multiple vaccines. And how are the gatekeepers managing that, Lieven?
Lieven Van der Veken: It has indeed become a very complex landscape. Because there’s a range of vaccines, you have to look for a set of vaccines that have higher efficacy against certain variants. Decision makers do start most often in my conversations with them from the perspective: does the vaccine confer protection against severe disease or death?
We have seen that the protection against severe disease for a number of the vaccines is actually higher than the protection against overall disease. There may be settings in which these vaccines no longer offer the 98 percent protection that perhaps was found in some of the clinical trials. These vaccines often continue to be incredibly important life-saving interventions in spite of what perhaps may sometimes be the narrative. Let’s not forget before this all started in October, November, the world was planning for a 50 percent efficacy of impact on severe disease of the vaccine.
The world was planning to celebrate 50 percent as efficacious and as something that should absolutely be recommended. So we may have gotten a bit spoiled with the incredible and beyond-expectation results of the first vaccines. Having said that, not only do we have these vaccines that are of very high efficacy and confer protection, but also, everybody does want to continue to access the vaccine that is most suited to their environment. That will continue to be a journey of understanding much better what is the virus that is circulating today.
We call certain variants the British variant, the South African variant, or a variant from some other place. But who knows whether that is where these variants originated? Our ability to detect variants is still very, very low. Our surveillance systems are still very, very weak. The first thing we need to do is really deepen our understanding of the circulating viral strains and detect new ones.
There is an exercise to match the vaccine candidates with the optimal environment in which to use them. I have to say there is a scenario. Today, it’s all about access to a vaccine, not just about access to the vaccine that is most suited for that environment. But in the next couple of months, we may see that dialogue shift.
Tania Zulu Holt: That is very interesting, isn’t it, Lieven? Because if you kind of play that out, it could even mean that maybe countries will need to exchange vaccines with each other so that they get access to the vaccine that’s the most suitable for the variants that might be at high circulation in their particular geography.
The other thing here is that increased collaboration is going to be critical to moving the world forward, in terms of the vaccines. But we’re also seeing that people want to think about when they can start traveling again—and about vaccine-certification documents and so forth. These things, of course, are only as valuable as the other countries that are willing to accept the documentation that you’re able to put together for your vaccinated population. So I think we’re also continuing to move into a phase of increased collaboration so that the countries can solve the pandemic together.
Lieven Van der Veken: I totally agree, Tania. And that points back to the old challenge that we discussed a few times, which is this incredible tension between optimizing for the best use of an individual vaccine dose and actually getting the biggest benefit across the world and actually trying to complete vaccination in individual countries, which is an incredible tension to work with. Because on one hand, we actually see incredible progress. COVAX [COVID-19 Vaccines Global Access] has brought vaccines to a large number of countries much, much faster and is scaling much, much faster than the closest historic precedent, H1N1 campaigns, was ever able to do, which is fantastic.
But at the same time, we actually do see countries that do not have access yet. And we do see continued pressure on these global allocations and global distribution mechanisms to find access to the dose and find access to the right doses. So the tension is live. It’s playing out every hour of every day in the world.
Diane Brady: So, Tania, I’m curious, what’s been the role of influencers in this campaign? You mentioned that it’s been important in previous ones.
Tania Zulu Holt: Absolutely. We can reflect back all the way to the polio campaign in the US when we had Elvis Presley taking a polio vaccine on national TV, or most recently in northern Nigeria where we’ve had the Emir of Kano giving the polio vaccine to children.
In this current pandemic, what we’ve seen is actually the politicians doing this. In most countries, the heads of states or the like have been on national TV showing that they’re going first. And then the second group of people have really been the healthcare workers, who have also been receiving many of the first doses. They have been part of also building trust in the vaccines.
Diane Brady: I know it’s hard, Lieven, to say if this is the beginning of the end or the end of the beginning. Nobody wants to play soothsayer. Yet many politicians and others out there are already breathing a sigh of relief and are starting to remove some of the restrictions to try and stop the spread of the virus. Can you give us some sense of where we are?
Lieven Van der Veken: So, Diane, I’m an optimist, right? But I do think it’s too early to say it’s the beginning of the end. Because there are still so many twists and turns that actually could happen. But what is a fact, and what you start seeing happening in certain environments, is that the vaccine does reset our relationship with the pandemic.
Diane Brady: Tania, any thoughts on that? Especially somebody who’s studied other public-health campaigns, anything that surprised you about this one?
Tania Zulu Holt: No, I’m an optimist, I believe, on this point as well. But I would say when we take some of the low- and middle-income countries, I think we have to acknowledge that the starting point for many of those countries is that COVID-19 isn’t the largest killer in those countries.
And there are many, many other priorities. And I think if nothing else, the pandemic has certainly brought health security, the importance of investing in strong health systems, to the forefront of the political debate, but also the general debate among the population.
And so as we continue to jointly fight this pandemic, I think we’ll also in many countries see a continued heightened awareness and focus on healthcare at large. And hopefully that means that we will not just tackle the disease burden of COVID-19, but also many of the other big killers in the world that we still have today, whether that’s malaria, TB, HIV, et cetera.
Lieven Van Der Veken: So it’s such an excellent point, Tania. And while, of course, a lot still needs to be said and written about the journey of adoption of vaccines and their protection, I do hope that, relatively fast, the most vulnerable will be protected from severe disease.
And that allows communities to find balanced solutions where the direct impact of COVID-19 is balanced with the indirect impact of COVID-19, which also has been enormous: the impact on psychological disorders, the impact on mental health, the impact on the broad health challenges, the incredible health backlog that is building up in many communities, the undiagnosed cancer treatments, the difficult social situations, the difficult situations in households leading to an increase of abuse in many settings. There are many, many, many elements of the indirect impacts of COVID-19. And if anything, if the vaccines can already help us reset that balance a little bit in the next couple of weeks and months, then that will be a major purpose in its own right.
Diane Brady: What lessons do you think we’ll take from this or have you taken from this?
Tania Zulu Holt: The key lesson that I have taken, and I think that I hope the world has also taken, is that collaboration really matters. We have rolled these vaccines to market, to patients faster than any other public-health intervention that we have ever seen before.
And we can still do better. And I’m convinced that we will do better. So as the world starts to evaluate what we’ve done well and what we could have done better, I’m very, very hopeful that, for the next potential outbreak pandemic, we will respond faster and at even larger scale. But then I think the underpinning learning from this is that it took collaboration between many different kinds of stakeholders to get to where we are today.
The COVID-19 vaccines are here: What comes next?
Lieven Van Der Veken: Tania, I could not agree more. I was in a different setting the other day. And someone was asked, “What does COVID-19 stand for to you?” And they said, “There’s a reason COVID-19 starts with ‘co.’ It’s the ‘co’ of collaboration.” Nothing of what we have seen, not the fast development, not the manufacture and scale-up, not the delivery that’s happening now, with all its challenges, would be possible without collaboration—collaboration between innovators, collaboration within a country, collaboration between countries. We can only hope, I can only hope, that that is what we’ll take away, and we will build a stronger, more collaborative global health system and ecosystem as a result of this.
Tania Zulu Holt: I think we should never forget that this has been a massive humanitarian tragedy that we’ve all lived through all over the world, since the beginning of 2020. It has taken a massive toll on people’s mental health. People have lost their jobs. People are missing the most basic act of being able to give a hug to your parents, to your loved ones.
So as much as part of this discussion, of course, becomes technical—we talk about the excitement of science and responsibility of speed, et cetera—we should never forget that this is also an opportunity for us to transition into the next normal.
We talk about the economic impact from people and businesses going under. But there’s also the human impact: the mental health, the other pieces of what makes our lives valuable that I think we are only starting to see, scratching, frankly, the surface of those. That’s also one of the reasons for the importance of this vaccine work.
Diane Brady: Lieven?
Lieven Van der Veken: My message would be to think ahead. Because every day or every week that we can actually reach protection of the vulnerable, and hopefully reach herd immunity, that will be the end of the pandemic. And that is so important, not just because of the lives that are directly affected by COVID-19, which has amounted to an incredible toll in the last year, but also for all the indirect effects.
My wife is a pediatrician. The number of times she comes home with really dramatic stories about the situations in which children find themselves as a result of the lockdown measures, as a result of the mental-health implications, is tragic. That is, I think, what should keep us all going, to try to do this as fast as we can, to scale as fast as we can, to actually try to alleviate that human suffering.
Diane Brady: Right. Lieven, as you were talking, I did hear occasional sounds of children playing. What I think about is how to get this next generation, the children, playing again and back to school. Hope really is, I think, such an important driver in society. Lieven, Tania, thank you very much for sharing your insights during a difficult time and a difficult time to certainly make predictions. So thank you for joining us.
Tania Zulu Holt: Thank you.
Lieven Van der Veken: Thank you, Diane.
Diane Brady: That was Lieven Van der Veken and Tania Zulu Holt. To get the latest updates on the vaccines, go to our special collections page on McKinsey.com, and also I’m Diane Brady. See you next time. Thank you for joining us.