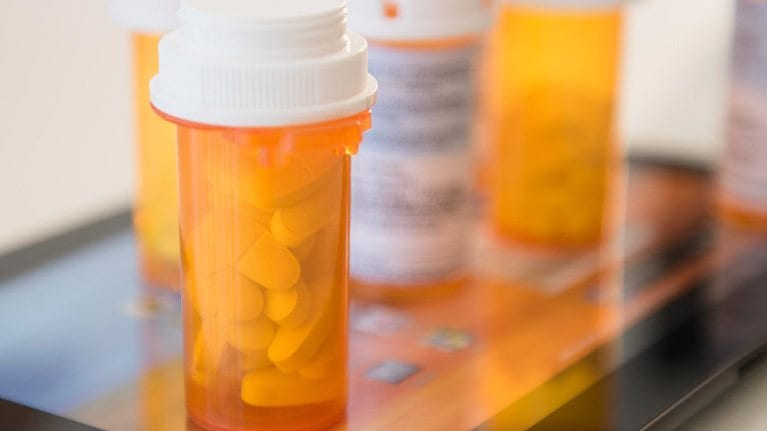
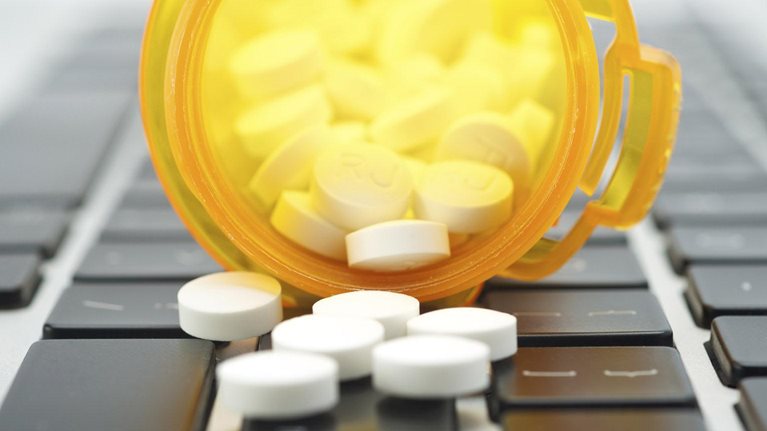
Consider the following: a 25-year-old, healthy male notices he is developing itchy, scaly patches of skin. He has not experienced anything similar before, so he goes online to do some research. Soon, he finds photos and descriptions that seem to match his symptoms and decides he has psoriasis. He pores over content in patient forums and reads strong views on which medications work best. He then makes a doctor’s appointment, and when the physician prescribes a typical ointment, he asks to be prescribed an injectable biologic instead, even though the physician feels his case is mild and is unsure his insurance company will reimburse the biologic.
Most—if not all—physicians practicing today in an outpatient setting have had similar experiences. We live in a world in which people naturally turn to their smartphones to look for price comparisons while shopping for electronics. It is similarly natural for them to seek information about their health the same way. One in twenty Google searches is now for health-related information.1

Would you like to learn more about our Pharmaceuticals & Medical Products Practice?
For the pharmaceutical industry, this presents a challenge. The traditional commercial approach based on mass-media advertising, hefty sales forces, ready access to physicians, and relatively uninformed patients is falling short. In particular, companies are failing to engage with patients in the early stages, when they look for information about symptoms. For example, a recent YouTube search for “psoriasis” produced among its top 100 results not a single branded video made by a pharmaceutical company. The first two videos had close to 500,000 views each. To connect with patients when they are looking for answers, pharma companies need to design a new approach based on an understanding of patients’ experiences and how they make decisions.
The healthcare decision journey, or CareFlow
Most pharmaceutical marketers are familiar with the concept of conducting market research to create a “sales funnel” as a guide for marketing programs, where patients move in stages from product awareness to product purchase. Often, these use a linear or sequential logic to represent patient behavior. In the retail industry, that linear journey has been augmented in recent years by the consumer decision journey (CDJ), which recognizes that in a world where consumers are empowered by information, the process involved in making a purchase is much more iterative (for more, see the article which revealed the concept, “The consumer decision journey,” McKinsey Quarterly, June 2009).
For pharma companies seeking to understand how consumers make healthcare decisions, the CDJ is enlightening. We now see consumers undertaking what we call a CareFlow (exhibit). A CareFlow maps a patient’s journey from the first awareness of a problem to treatment, examining the factors guiding their decisions at each stage. These insights enable pharma marketers to engage with patients in ways that feel natural and personal. That may mean providing information to help an important choice to be made, supporting the execution of that choice, or simply empathizing. For while the moment a prescription is filled at the pharmacy is the “success event” commercially, it’s just one of many points of influence in the CareFlow, alongside patients’ own research, their consultations with others, considerations of the cost of treatment, scheduling of appointments, responses to side effects, or remembering to take medications. Some may be far more important than the fulfilling of the prescription, such as the moment before the first time the patient self-injects a biologic (or the moment before the second time, when the patient remembers how much the first injection hurt). Every point in the CareFlow is potentially a vital point of interaction; by understanding it, the marketer can understand the relative importance of points and (re)allocate investment and attention accordingly.

The CareFlow also vividly illustrates the considerable branching and looping that can happen within each of five stages of a typical patient journey. The first group of instances relates to a patient’s recognition of a problem (what we call the external trigger). The second is the process the patient goes through to gather information. The third represents the patient beginning to evaluate treatment options (which can be iterative). The fourth is the beginning of treatment. And the fifth is the ongoing treatment. Patient behaviors and experiences at each point differ by disease, and even by patient, of course, so the CareFlow has to be disease specific. For example, a CareFlow analysis of a sample of psoriasis patients in the United States found that 58 percent had requested a specific brand of medication from their physician in the past year. This is twice as high as would be expected in the general patient population and illustrates the importance of communicating with certain segments of psoriasis patients before they visit a physician.
How pharma can win in a digital world
A CareFlow for depression built from a survey of more than 1,200 patients revealed how long it took for them to seek care. Although a diagnosis for depression can be made after 2 weeks of symptoms, 71 percent of respondents took more than a month to receive a diagnosis after first sensing something was wrong, and 38 percent took more than six months. The time lag represents an opportunity for pharma companies to accelerate the patient path to care. The CareFlow also revealed how better management of patients’ expectations—perhaps before as well as when they visit a physician—could improve adherence to treatment. Although the literature suggests that changes may be considered after 2 to 4 weeks of treatment, it also states that antidepressants can take 6 to 12 weeks to take full effect; providers typically wait this extended period before making a determination of a medication’s effectiveness.2 The survey, however, showed that 18 percent of prescribed medications were discontinued in less than one month and, in these cases, 52 percent cited perceived lack of efficacy as a reason.
CareFlows can be constructed using surveys of patients and physicians, and analysis of the data available on social media and from web-engine search trends, for example. Pharmacy claims, electronic medical records, and consumer data can also help build a comprehensive and more quantitative view of the patient flow. Data sets can include factors directly related to specific health conditions, as well as demographics, consumer behavior, and communications preferences. Lack of data will not be an issue.
CareFlows are an important new concept for helping pharma companies play a meaningful role in the decisions patients and healthcare providers make about care, ensuring their marketing tactics and offers are targeted, dynamic, and effective. Once companies are committed to understanding them, the next imperative is to reshape their commercial approach accordingly—something that is likely to require a reallocation of marketing focus and investment. In a digital world, they will be a crucial element of any successful commercial strategy.
For more on how digitization is revolutionizing the relationship between patients and pharma, and how companies can respond, see “Pharma 3D: Rewriting the Script for Marketing in the Digital Age,” Pharma 3D, April 2016.